Rabies: India
This is a collection of articles archived for the excellence of their content. |
Contents |
Immunisation
How does the vaccine work?
Jacob Koshy, Sep 10, 2022: The Hindu
Which virus causes rabies? What is the treatment protocol?
How does a rabies vaccine work?
Rabies is a disease that is caused by a family of viruses called the lyssaviruses and found in a range of mammals. The virus targets the central nervous system and is nearly 100% fatal to the host animal if it succeeds in infecting it. Though many animals from cats to crocodiles can be transmitters of the virus, it is most likely to spread to people from the bite of an infected dog or a cat as they are the most common pets. Despite being potentially lethal, the virus is slow-moving and it can be several weeks before the disease manifests into a fatal encephalitis which is why administering a vaccine, even after being bitten by a rabid animal, is effective. A shot of rabies immunoglobulin (rabies-antibodies against the virus derived either from people or horses) followed by a four-week course of anti-rabies vaccine, is nearly guaranteed to prevent rabies. This translates to the first dose being given on the same day as the immunoglobulin followed by vaccinations on the 3rd, 7th and 14th day. There are other regimens, such as five shots which include one on the 28th day approved by the World Health Organization (WHO) which clinics may consider, depending on the availability of the vaccine.
How is the vaccine made?
The vaccine is made up of an inactivated virus that is expected to induce the body into producing antibodies that can neutralise the live virus in case of infection. There are also test vaccines that involve genetically modified viruses. There is no single-shot rabies vaccine or one that offers permanent immunity. There are mainly two ways of administering the rabies vaccine. One, called post-exposure prophylaxis (PEP), is given to persons who have been exposed via a bite to an animal suspected to be infected. The vaccines are administered either into the muscles, or into the skin. It can also be given ahead of time to persons who have a high risk of being infected, such as veterinarians, animal handlers, areas with a high number of rabies infection, by what is called Pre Exposure Prophylaxis (PrEP). The advantage of a PrEP is that if bitten, one doesn’t need a immunoglobulin injection, and two subsequent shots of the vaccine will suffice for full protection, unlike the four-course prescription in the case of PEP. However, the WHO doesn’t recommend PrEP as a general preventive.
Are rabies vaccines easily available in India?
According to the Health Ministry, there are at least six rabies vaccines approved for India. They all contain inactivated virus made of duck, chicken or human cell cultures and are marked as safe, efficacious and with long immunity. Rabies vaccines are available for free in government dispensaries though vaccines administered in a private clinic can cost up to ₹500 per dose. However, reports of hospitals running out of vaccines continue to surface and knowledge about vaccines and treatment is still inadequate in India. The Health Ministry has said that no centralised database of vaccine availability is maintained, being a State-procured product, but that shortage had been reported in Punjab, Haryana, West Bengal and Karnataka. The Centre says that from 2016-18, around 300 laboratory-confirmed rabies deaths were reported in India. The WHO says India is endemic for rabies and accounts for 36% of the world’s deaths. The true burden of rabies in India is not fully known; although as per available information, it causes 18,000-20,000 deaths every year. About 30-60% of reported rabies cases and deaths in India occur in children under the age of 15 years, as bites that occur in children often go unrecognised and unreported, it notes. What about vaccines for animals?
Given that rabies treatment requires multiple shots of vaccine as well as immunoglobin, sticking to the schedule is challenging. Governments of countries where rabies is endemic have frequently set targets to eliminate the disease — India has committed to do so by 2030. Yet it is widely acknowledged that this elimination requires vaccination of dogs. Like in people, vaccinating animals too doesn’t guarantee lifelong immunity from the disease. Because dogs are deemed responsible for 99% of all rabies infections in people, the government in its 2021 plan, called the ‘National Action for Plan — Rabies Elimination’, aims to vaccinate at least 70% of all dogs in a defined geographical area annually for three consecutive years. With this, a degree of herd immunity is expected leading to eventual elimination within eight years. Rather than inoculate all dogs, the plan is to identify ‘rabies hotspots’ in the country and target them.
Rabies immunization protocol
Asit Jolly , Homegrown cure for Rabies gets WHO nod “India Today” 12/2/2018
The World Health Organization (WHO) has notified a rabies immunisation protocol developed by Omesh Bharti, 49, a government doctor in Himachal Pradesh, as the new global standard. The procedure, successfully tested on thousands of dog and monkey bite victims in the past five years, brings down the cost of treatment from Rs 35,000 to Rs 350 per patient!
The existing treatment involved injecting patients with the rabies vaccine and rabies immunoglobulin (RIG) extracted from horse or human blood. Human RIG, which needed to be administered in large doses as per the victim's body weight, cost Rs 6,000-8,000 per vial, and was "beyond the reach of most victims". Working at the time (2013-2015) as a health officer with the Shimla Municipal Corporation, Bharti had rare access to brain tissue samples from rabid dogs, monkeys and Himalayan palm civets found dead in the area. He evolved a protocol that required a fraction of the RIG needed for conventional treatment. "A tiny amount of RIG injected directly into the wound was just as effective as administering large amounts," he says. Similarly, administering 'intra-dermally' rather than as an 'intra-muscular' injection required less than a 10th of the vaccine. Despite early scepticism, the meeting of WHO's Strategic Advisory Group of Experts (SAGE) in Bangkok in 2016, included Bharti's protocol in its agenda for discussion. "By then, we had 7,000 successful cases in Himachal," he says.
It helped that Himachal health authorities avidly supported Bharti's work. Even before WHO's endorsement, Bharti has trained scores of local medical professionals deployed at myriad state-run rabies clinics across the state. Himachal has now made rabies treatment (using RIG) free.
"In 2017, there were just two rabies-related deaths [in HP]-one a woman who refused treatment; the other a youth who went to a private practitioner," says Bharti. His work could help stem substantially the 55,000 rabies deaths a year reported worldwide, the majority in Asia and Africa.
Finally endorsed by the SAGE in Geneva on January 15 as "cost-, dose- and time-sparing, while assuring safety and clinical effectiveness", the updated WHO recommendations on rabies immunisation supersede its 2010 position. A full version of the new protocol is in cue for publication in the Weekly Epidemiological Record in April.
Goa
2021: first state to eliminate rabies cases
Nida Sayed, June 26, 2021: The Times of India

From: Nida Sayed, June 26, 2021: The Times of India

From: Nida Sayed, June 26, 2021: The Times of India
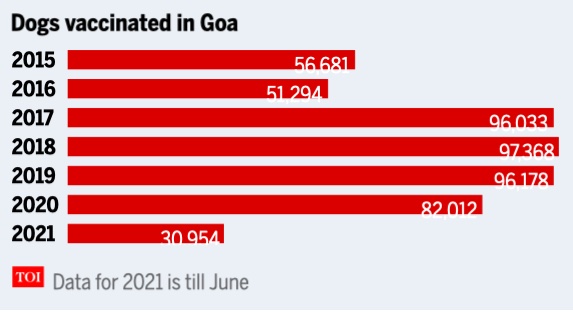
From: Nida Sayed, June 26, 2021: The Times of India

From: Nida Sayed, June 26, 2021: The Times of India
In 2018, Goa recorded zero cases of people getting rabies after being bitten by a dog in the state. It maintained the record in 2019 and did it again in 2020. As of June 2021, there have been zero human rabies cases in the state for over three years and just eight cases in which dogs were found to be infected. Goa officially became the first state in India to beat the virus, in a country that sees an estimated 45 lakh cases of people being exposed to rabies annually.
“The state-wide rabies control in Goa has been the result of a global collaborative effort,” the organisation Mission Rabies said in a celebratory post on its website on June 23. The achievement stands out because India accounts for 36% of all the deaths in the world due to rabies and up to 20,000 people die annually due to it, says the World Health Organisation.
According to the global health body, about 30-60% cases and deaths are seen among children under the age of 15, since dog bites are either unrecognised and unreported. In 2018, the WHO launched a global strategic plan to eliminate dog-mediated human rabies by the year 2030.
Goa’s achievement was the result of a seven-year campaign that involved the state’s directorate of animal husbandry and veterinary services (AHVS) and the Mission Rabies, an initiative founded by the UK-based Worldwide Veterinary Service.
A mass vaccination campaign
In 2014, Mission Rabies began its surveillance of rabies cases after getting a positive response from the state government. The organisation responded to 45 cases, in which 39 of the dogs tested positive. As surveillance across the state increased, the number of rabies cases that came to light rose.
The organisation discovered there was no data available on the total number of stray or pet dogs, and there was no estimate of dog deaths due to rabies. As a result, the first stage of the project focussed on an assessment of the dog population, the funds required to vaccinate them and formulating a plan.
Led by Mission Rabies founder and CEO Luke Gamble, a team of volunteers decided to vaccinate 50,000 dogs in 30 days. Over 500 veterinary doctors from 16 different countries arrived in the state to assist local veterinarians and dog catchers. It was a success. Exceeding their target, the volunteers vaccinated 63,000 dogs in 30 days.
Having got a rough idea of Goa’s stray dog populace, lengthy discussions were held with local veterinarians and AHVS officials. Following that, the Manohar Parrikar-led state government in 2015 signed an MoU with Mission Rabies to carry out a dog vaccination drive across the state.
As a result of this agreement, rabies vaccines have been administered free of cost to dogs in Goa since 2015. The state government has spent Rs 3.48 crore till August 2020 on rabies control.
“Parrikar had the vision to realise that if we focus on the problem, have faith in the team and divert funds towards the project, the elimination of the rabies virus is possible,” said Gowri Yale, scientific and technical manager at Mission Rabies.
The battle against rabies
The organisation set up a 24-hour rabies surveillance system, which included a hotline number for citizens to report suspected rabies cases. Teams of volunteers would visit each taluka to vaccinate and sterilise dogs. A rapid response and support team were also set up to help dog bite victims in the state.
After awareness about rabies was found to be very low among children in 2014, Mission Rabies started campaigns to educate students in 1,450 schools about avoiding and the management of dog bites. Till date, 5.4 lakh rabies vaccinations have been administered to dogs, and nearly 10 lakh students and citizens have been educated in awareness campaigns.
The awareness programmes continued during the Covid-19 pandemic through online videos that were shared with schools.
Animal rabies cases remains a worry
Despite detecting no cases of persons with rabies since 2018, Goa isn’t 100% rabies-free. Even in 2018, the one rabies death recorded was of a boy from Sawantwadi taluka who was bitten by a dog outside the state. “Animal rabies cases are detected from time-to-time at border talukas only due to migration from unprotected Maharashtra,” said Murugan Appupillai, Mission Rabies’ education director.
He said that Maharashtra was “flooded with rabies cases” that are not reported or recorded. The state government has written to Karnataka and Maharashtra about the issue but has received limited response so far.
The stray dog populace from neighbouring states was a particular matter of concern following the national lockdown in 2020.
“Many dogs migrated into Goa in search of food (during the lockdown) and we suspect that this was the reason for an increase in rabies cases among stray dogs. These cases were mainly reported in Bicholim, Pernem and Sattari making it a total of 24 rabies cases last year,” said Yale.
Braving the rain after the lockdown, teams of volunteers spread out across the state and managed to restrict the number of cases. To their relief, there was no case of a person being infected in the state.
The AVHS announced on June 23 that people entering Goa with pets, especially tourists, had to inform them about the number of animals and their vaccination details using the anti-rabies hotline (+91 7744029586).
“If their pets are not vaccinated, we will arrange for the vaccination free of cost,” said Dr Marvin Lopes, AHVS deputy director and nodal officer for Mission Rabies in Goa.
The state government is optimistic that they can monitor pets brought by people, but the control of stray dogs remains a matter of concern. The aim is to now vaccinate stray dogs in the Maharashtra-Karnataka border areas and thus prevent potentially rabid dogs from entering Goa. Mission Rabies is also going to take up a rabies vaccination campaign in September-October to ensure dog owners vaccinate their pets.
"We will be joining hands with NGOs and animal rescuers across Goa to help us with the campaign,” said Julie Corfmat, Mission Rabies project manager.
"This campaign will be launched on world rabies day, on September 28 and will go on till October 14. The proposed schedule for the campaign will focus on one taluka per day." she said.