Muzaffarpur (after 1947)
This is a collection of articles archived for the excellence of their content. |
Contents |
State of health
AES cases, 2010-18
Rema Nagarajan, June 22, 2019: The Times of India

From: Rema Nagarajan, June 22, 2019: The Times of India
See graphic:
Muzaffarpur- AES outbreak, Number of cases and number of deaths, 2010-18
As in 2015-16
Sushmi Dey, June 20, 2019: The Times of India
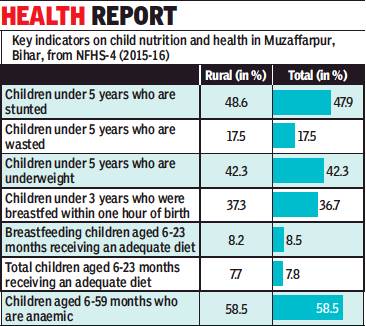
From: Sushmi Dey, June 20, 2019: The Times of India
Lychee toxins, malnutrition, heat wave or poor health infrastructure – what is causing the encephalitis related child deaths in Muzaffarpur? Even as the state government blames hypoglycemia as the cause for most deaths, doctors, public health experts and researchers have raised concerns over the government’s failure to contain the rapidly rising toll.
This has also compelled the health ministry to send different teams to probe and ascertain the exact cause. Ten paediatricians and five para-medics from RML Hospital, Safdarjung and Lady Hardinge Medical College are part of the five teams set up. The teams also include clinical and public health experts from Indian Council of Medical Research (ICMR), National Institute of Nutrition and UN agencies.
“As of now, we do not have much clue about the exact cause of these deaths. However, we are hopeful of zeroing on it in a day or two,” a senior official from ICMR told TOI.
Though lychees are being seen as a primary cause, researchers say the fruit can only be a contributing factor. Instead, prolonged malnourishment, the current heat wave, poor hygiene and lack of awareness about lychee consumption may have led to the deaths.
“There is a particular component in the fruit which can contribute to reducing blood sugar level if too many lychees are consumed in an empty stomach,” said a public health expert. Official data suggest the Bihar government has been indifferent towards improving child nutrition and healthcare in this district.
In Muzaffarpur, nearly 48% children under the age of 5 are stunted, 17.5% are wasted (too thin for their height), while 42% are underweight, according to the National Family Health Survey (NFHS)-4. “Patients from villages are rushing to town to seek treatment at tertiary care and losing time in the process. If they go to the nearest health centre or clinic, they can get immediate care and the situation can be controlled,” another health expert said.
As in 2019
Rema Nagarajan, June 20, 2019: The Times of India
While the state and Union governments are now scrambling to deal with the outbreak of acute encephalitis syndrome (AES) disease in Bihar’s Muzaffarpur, official data shows the shocking state of the public health infrastructure in the district. The health ministry’s health management information system (HMIS) shows that all of the 103 primary health centres (PHC) and the only community health centre in the district were not considered even fit for evaluation or were rated 0 out of 5.
The mandatory requirements for a PHC to be evaluated under HMIS were that if it is a 24x7 centre, it has to have at least one medical officer, over two nurse-midwives and a labour room. For non-24x7 centres, all that was needed was at least one medical officer and one nurse. Yet, 98 of the district’s 103 PHCs could not meet even these minimum requirements and hence were not graded in the 2018-19 evaluation.
Muzaffarpur should have 170+, not just 103, PHCs
At least 98 of Muzaffarpur district’s 103 primary healthcare centres (PHCs) could not meet even minimum requirements. Of the remaining five, every single one got a zero rating. The rating consists of three points for infrastructure and two for services. Thus, each of the five failed miserably on both counts.
Incidentally, according to the official norms, there is supposed to be one PHC for every 30,000 population in the plains. By that count, Muzaffarpur should have had over 170 PHCs for its population of a little over 5.1 million.
The situation of the lone community health centre (CHC) was no better. In the 2017-18 rating of CHCs, the one in Muzaffarpur was rated “not eligible”. This is because it failed to meet the mandatory criteria required for being rated.
What were these mandatory criteria? In terms of staffing, there should have been two or more doctors, six or more nurses or ANMs (auxillary nurse-midwife) and at least one lab technician. As for infrastructure, there should be an operation theatre, a generator and separate “public facilities” (read toilets) for men and women.
Again, Muzaffarpur’s population should have meant it should have at least 43 CHCs, given the norm of a CHC for every 1.2 lakh population in the plains. Instead, there is just one and that in a shape that does not even merit evaluation. What makes this situation particularly shocking is that the district has been witnessing deaths of scores of little children at this time of the year every year for the last two decades or more. And yet, successive governments have not bothered to beef up the public health infrastructure to cope with even routine health needs, leave alone a medical emergency they know will hit unfailingly each year.
SKMCH ‘paediatric ICU’ unfit for tag
The central team that probed the death of children from AES in Muzaffarpur stated that the paediatric ICU of Sri Krishna Medical College and Hospital (SKMCH) did not meet the criteria to qualify as a paediatric ICU. It said mortality from AES usually ranges from 6-19% in good centres. In SKMCH, mortality rate has been about 25% this year.
2019, June
Rema Nagarajan, June 22, 2019: The Times of India
Abandoned Till The Predictable Crisis Hits
Doctors, ambulances rushed to fight disease only when the spotlight’s on it
Rema.Nagarajan@timesgroup.com
Vaishali/Muzaffarpur:
As the Bihar administration heaved a sigh of relief with the day’s AES death toll falling to five in the state on Friday and over a 100 admitted children being discharged, the village of Harivanshpur, which has seen the largest number of deaths for a single village — 11 till date — is still holding its breath.
Ever since one family lost three siblings within a couple of days, there is intense fear in Harivanshpur. People have packed their children off to their in-laws’ villages out of fear that something in the air or water was causing it. Parents are watching their children like hawks and yet kids continue to fall ill. Not all may be due to AES, but every child with even the slightest fever is being rushed to the nearby spanking new Bhagwanpur Community Health Centre as parents are scared to take a chance.
With intense focus from Delhi and Patna, most state health facilities in and around Muzaffarpur, the epicentre of the AES outbreak, have received additional staff and ambulances, deputed from neighbouring areas.
The entire area is now swarming with ‘teams’ from Delhi and Patna, including doctors, epidemiologists, microbiologists and health researchers from premier research institutes such as the National Institute of Virology, Indian Council for Medical Research, National Centre for Disease Control and so on. The deployment of greater resources and following of a strict protocol in treatment may have helped reduce the mortality significantly.
Sadly, none of this urgency existed even a fortnight back when the epidemic took off with a sudden spike in AES cases and deaths, though the first officially acknowledged AES death was registered as early as April
29. Whether in Sri Krishna Medical College and Hospital (SKMCH) or in primary health centres, there is an acute shortage of staff at all levels. In fact, the biggest lacuna in the system, even more than infrastructure or availability of medicines, is the non-availability of doctors, nurses, pharmacists, lab technicians and health workers. Sanctioned posts of every kind and at every level in the health system lie vacant in Bihar in general and Muzaffarpur in particular.
“We are supposed to have six doctors in this 24x7 PHC. We have only three. The government has given an Ayush (alternate medicine), a homeo and a dentist and said, ‘there, you now have six’. But patients refuse to consult them. Then what use are they?
Interestingly, Muzaffarpur has the highest concentration of doctors in that part of Bihar, but few of them are working for the government. According to the former secretary of the Muzaffarpur chapter of the Indian Medical Association, Dr Sanjay Kumar, it has about 800 members. “There must be about 500 in that 1.5 kilometre stretch of Juran Chapra alone,” said Dr Kumar, referring to the Harley Street of Muzaffarpur, which is packed with MBBS doctors and specialists of all hues in every lane and bylane not to mention nursing homes, diagnostic labs and the like. Similarly, Muzaffarpur has two nurse training centres attached to the medical college and the district hospital. Yet, most public health facilities have a shortage of nurses.
Despite all its limitations, though, there is only the public health system when it comes to an outbreak of this sort. Private hospitals in the city empanelled under the Ayushman Bharat scheme have not shown any eagerness to take in AES patients. The exception is the Kejriwal hospital that is treating them free of cost but not under the government scheme.
The medical college superintendent is elated that the government has promised to expand it to 1,500 beds from the current 600. However, the reality is that it is a struggle to find enough doctors even for 600 beds.
Deaths have crossed 145 out of the 600-plus AES cases this season. Though the causes are being debated, there is unanimity that the treatment protocol is the same no matter what the cause and that timely access to proper quality treatment could ensure much better survival rates.
“There is one sure-fire underlying cause in all cases; that’s poverty. As a preventive measure, the government could work on ensuring no family is poor. Can it do that?” asked a senior doctor rhetorically in response to charges that the public health system hadn’t taken enough preventive steps to counter AES.