Mental health: India
This is a collection of articles archived for the excellence of their content. Additional information may please be sent as messages to the Facebook community, Indpaedia.com. All information used will be gratefully acknowledged in your name.
This is a collection of articles archived for the excellence of their content. |

Depresssion
2016: Prescriptions increase 14%
Malathy Iyer, Prescriptions for major depression up 14% in '16, Jan 30, 2017: The Times of India
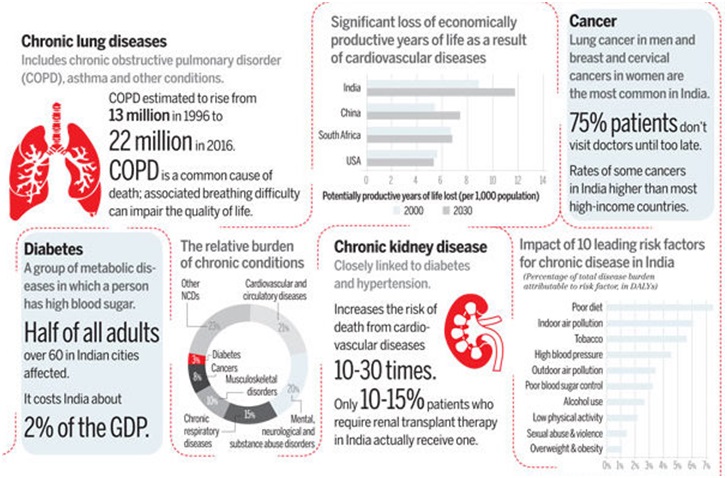
Indians popped more anti depressants in 2016 than ever before, indicating perhaps that they are now more open to the idea of seeking help for mental health problems. Around 10.6 lakh more prescriptions for anti-depressants were written in 2016 than in 2015, shows data collated by health information agencies. While 3.35 crore prescriptions (for new patients) were written in 2015, doctors wrote 3.46 crore new prescriptions in 2016.
The number of prescriptions written out only by psychiatrists in 2016 represented a 14% rise over 2015. Psychiat rists treat patients with major depressive disorders while doctors from multiple specialties treat patients with mild or disease-related depression. Depression, though widely spread in India, is rarely given importance in the public health system, which is burdened by infectious diseases such as tuberculosis and dengue as well as noncommunicable diseases such as diabetes and hypertension.In October 2016, the National Institute of Mental Health and Neurosciences in Bengaluru released a mental health survey that said one in every 20 Indians suffered from some form of depression. The prevalence of depression across the world has increased to such an extent that it's the theme for the World Health Organisation's World Health Day on April 7.
When contacted, NIMHANS director Dr B N Gangadhar said the increase in prescriptions could also be an indication of the increasing number of psychiatrists in India. “There is no doubt that people are more open than before to seek help for depression, but a 14% rise in prescriptions could also mean there are more psychiatrists today than before,“ Dr Gangadhar said.
2017: the ailments of 1/7 of Indians
Durgesh Nandan Jha, Dec 24, 2019 The Times of India
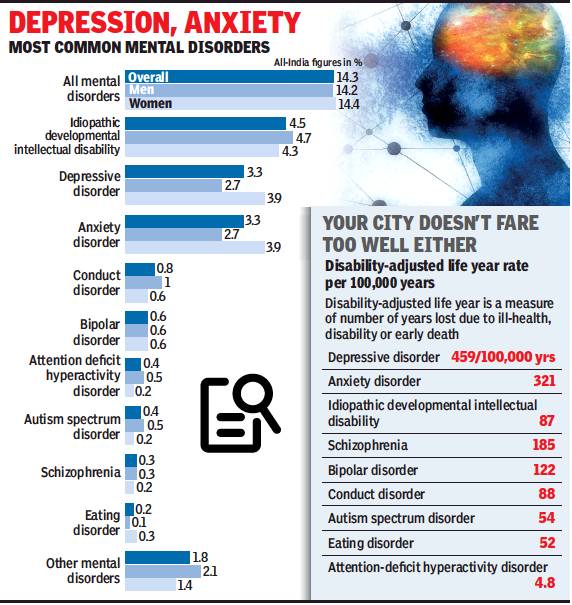
Depression and anxiety disorders are the most common mental disorders and their prevalence is increasing across India, a study published in the Lancet Psychiatry shows.
According to the study findings of which were released on Monday, 197 million Indians (14.3% of the total population) were suffering from mental disorders in 2017. Of this, 46 million people had depression and 45 million were having anxiety disorders.
In Delhi, life year lost to death or lived with disability due to depressive disorders and anxiety disorders was calculated to be 459 years and 321 years, respectively, in an average of 1,00,000 years.
Dr Rajesh Sagar, professor of psychiatry at AIIMS, said stress is a leading cause of both depression and anxiety disorders. “Among children, bullying mainly led to the two mental disorders,” he added.
According to Dr Sagar, because of the changing social milieu mechanism to cope with these illnesses is also affected. “Earlier, in joint families, much of the stress and anxiety was relieved because there were people to share one’s problems with. But now most families are nuclear,” he said.
Across India, the contribution of mental disorders to the total disease burden in India in terms of the disabilityadjusted life years (DALYs) increased from 2.5% in 1990 to 4.7% in 2017. Mental disorders were the leading contributor in India to years lived with disability (YLDs), contributing 14.5% of all YLDs in 2017.
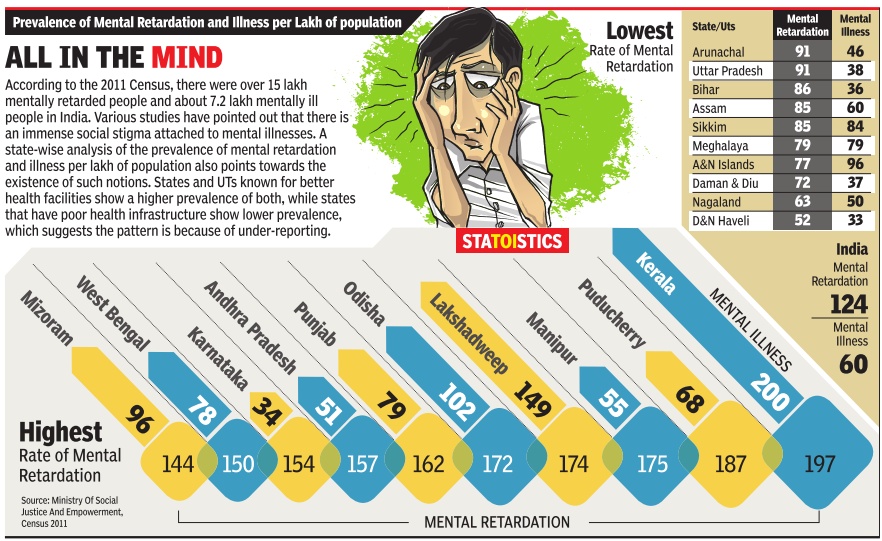
The prevalence of depression is the highest in older adults, the doctors said. The state-specific findings published in the Lancet Psychiatry also highlight the extent of the effort needed in each state to address mental health which could serve as a reference for policy makers to plan approaches for reducing the growing burden of mental disorders in a systematic way.
“The prevalence of adult mental disorders is higher in the southern states and that of childhood onset mental disorders is higher in the northern states, said professor Balram Bhargav, director general of Indian Council of Medical Research (ICMR), citing the findings of the research.
“Given the significant contribution of mental disorders to the disease burden in India, further research should continue to track the changing trends of mental disorders in different parts of the country,” he added.
Dr Lalit Dandona, director of the India State-Level Disease Burden Initiative, said the high rate of depression among the older adults reported in this study is of concern and needs attention. The significant association of suicide with depression emphasises the need to identify and deal with depression through wider efforts in the community and in the health system.
“Mental illnesses contribute significantly to the burden of disease in India as reported by this study. There is an urgent need to strengthen mental health services, integrate these with general healthcare, and remove barriers such as stigma and access to treatment.”